
Medical Director
Senior Consultant, General & Colorectal Surgeon
MBBS (Singapore), MRCS (Edinburgh), MMed (Surgery), FRCS (Edinburgh)
What is Colorectal Cancer?
Colorectal cancer is the most common cancer in Singapore for both males and females combined. Early detection requires regular screening as well as prompt medical consultation should symptoms occur.
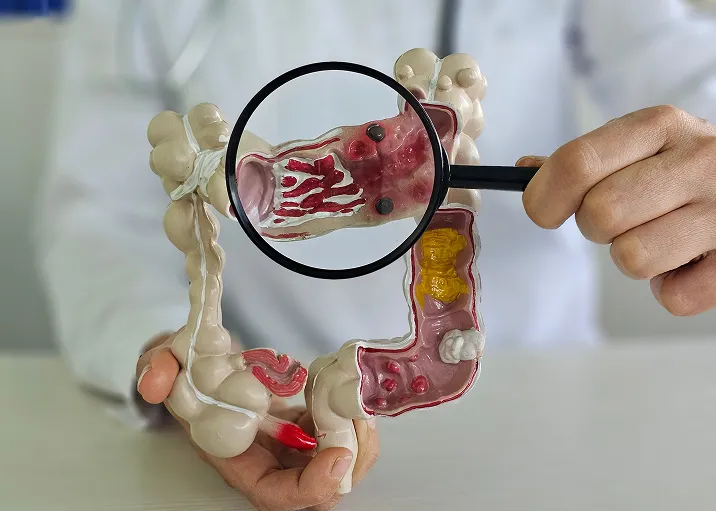
Also known as bowel cancer or colon cancer, this type of cancer occurs when cells in the colon or rectum grow abnormally and uncontrollably, developing into tumours.
Most colorectal cancers begin with benign growths (polyps) in the inner lining of the colon or rectum. Over time, these polyps can progress, invade the surrounding tissues, and, in advanced stages, spread to surrounding tissues and organs.
Symptoms of colorectal cancer can be variable and non-specific, but most commonly include:
- Changes in bowel habits (e.g. increased diarrhoea or constipation, pencil-thin stools, increased urge to pass motion)
- Blood in stools
- Weight loss, reduced appetite
- Abdominal pain
- Feeling of lethargy, tiredness or getting breathless with activity may suggest anaemia with blood loss that is not obvious to the eye
What are the Risk Factors for Colorectal Cancer?
Several factors can contribute to an increased risk of colorectal cancer.
These include:
- Being over the age of 50
- Personal or family history of colorectal cancer or polyps
- Smoking
- Heavy alcohol consumption
- A diet low in fibre and high in red meat, processed meat, and fats
- A sedentary lifestyle
- Being obese or overweight
Can Colorectal Cancer be Prevented?
The most effective approach to preventing colorectal cancer is through early detection and preventive screening. For individuals without any risk factors besides age, the recommended age for screening starts at 50. However, those with a family history of the disease or who have other risk factors, should begin screening earlier.
Besides regular screening, adopting a healthy lifestyle may lower colorectal cancer risk. This includes consuming a healthy and balanced diet, refraining from smoking, reducing alcohol intake, staying active, and ensuring a healthy weight.
How is Colorectal Cancer Diagnosed?
There are a few screening tests available for colorectal cancer in Singapore:
Colonoscopy
- A colonoscopy allows doctors to examine the lining of the colon and rectum using a flexible tube with a camera. Polyps can be detected and removed during the procedure, making it both diagnostic and preventive. It is considered the gold standard for colorectal cancer screening and only needs to be repeated every 10 years if no polyps or other risk factors are present.Faecal Immunochemical Test (FIT)
- The FIT is a non-invasive test that checks for hidden blood in the stool, which can be an early sign of colorectal cancer. While it is more affordable and convenient than a colonoscopy, it is less accurate and needs to be done every year.Imaging Tests
- CT and MRI scans provide detailed images of the colon and surrounding tissues. These imaging techniques are typically used to evaluate abnormalities found during other tests or to assess the extent of tumour spread.Sigmoidoscopy
- Similar to a colonoscopy, a sigmoidoscopy uses a flexible tube to examine the rectum and lower part of the colon (sigmoid colon). While a sigmoidoscopy does not examine the entire colon, it can still be effective in detecting cancer or polyps in the lower intestinal tract.Barium Enema
- A barium enema is an X-ray examination of the colon and rectum. The colon is filled with a contrast dye (barium solution) to improve image clarity, allowing doctors to spot abnormalities such as growths or structural changes.
What are the Stages of Colorectal Cancer?
The stages of colorectal cancer are determined by the extent of its spread using the tumour, node, and metastasis (TNM) staging system. Staging helps determine the appropriate course of treatment and prognosis for patients.

Stage 0
Also known as carcinoma in situ, the cancer is located within the inner layer of the colon or rectum.

Stage 1
The cancer has progressed beyond the inner layer, but not into the colon or rectum wall.

Stage 2
The cancer has developed within the colon or rectum wall, but has not spread to nearby lymph nodes.

Stage 3
The cancer has metastasised to the surrounding lymph nodes.
Stage 4
Cancerous growths are present in surrounding tissues and organs, such as the liver, lungs, or bones.
When to see a Colorectal Cancer Doctor
Should you experience persistent symptoms such as bowel habit changes, blood in stool, or abdominal discomfort for longer than two weeks, it is recommended to schedule an appointment with a colorectal cancer doctor. These symptoms may indicate early-stage cancer or another severe condition requiring prompt medical attention. Additionally, individuals with a family history of colorectal cancer are at greater risk and are advised to undergo earlier and more frequent screenings.
Monitoring the frequency and severity of symptoms can provide valuable information to a doctor for determining an accurate diagnosis and an appropriate treatment plan for colorectal cancer.
How is Colorectal Cancer Treated?
After detailed staging investigations are done, surgery is needed for a definitive cure. Colorectal cancer surgery will remove the affected part of the intestine, lymph nodes around the tumour, and possibly surrounding organs if the cancer has invaded or involved these structures.
Dr Chew Min Hoe will tailor a colorectal cancer treatment plan based on the stage and severity of the disease. Surgery techniques can include open surgery or laparoscopic (minimally invasive) surgery. The aims of surgery will be to ensure complete cancer clearance, low complication rates, as well as good and enhanced recovery.
Open surgery for colorectal cancer
involves making a long abdominal incision to access the tumour, nearby lymph nodes, and other affected structures. This is more commonly performed for advanced or complex cases of colorectal cancer and involves a longer hospitalisation and recovery.
During laparoscopic surgery
on the other hand, the colorectal cancer surgeon makes several small abdominal incisions (0.5-1 cm) through which a long, thin tube called a laparoscope and other specialised surgical instruments are inserted. It allows the surgeon to visualise the abdominal cavity on a monitor and remove the diseased portions of the colon or rectum. Compared to open surgery, this procedure provides reduced discomfort and a shorter recovery time.
Common types of colorectal cancer surgery include:
Partial Colectomy - Only the cancerous portion of the colon and some surrounding healthy tissues are removed, while the remaining parts of the colon are reattached.
Total Colectomy - This procedure involves the removal of the entire large intestine while the small intestine remains attached to the rectum.
Ileocolectomy - The affected ileum segment will be removed, while the remaining parts of the small intestine will be sutured together.
Abdominoperineal Resection - This procedure removes the rectum, anus, and parts of the sigmoid colon.
Proctosigmoidectomy - This involves the partial or complete removal of the sigmoid colon and rectum.
Total Proctocolectomy - This form of colon cancer surgery removes the entire large intestine and rectum.
Chemotherapy and radiotherapy may be required as part of the treatment and these will be coordinated with medical and radiation oncologists, along with targeted treatment specific to your cancer, in order to achieve the best possible outcomes.
What are the Side Effects of Colorectal Cancer Treatment?
Patients undergoing colorectal cancer treatment may experience a range of side effects depending on the chosen treatment approach.
Surgery is a common treatment for colorectal cancer, particularly in its early stages. While often effective in removing cancerous tissue, surgery can lead to pain, infection, changes in bowel function, and temporary digestive concerns.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells, but it can also lead to unwanted side effects such as nausea, fatigue, hair loss, skin reactions like rashes, and flu-like symptoms.
Radiation
Radiation therapy targets cancer cells with high-energy rays. While effective, it can cause skin changes, fatigue, localised hair loss, and digestive issues.
Side effects from colorectal cancer treatment can take a toll. But with the right support, medications, and lifestyle changes, many of these symptoms can be managed more comfortably. Before undergoing such treatments, it is crucial to discuss possible adverse effects with a doctor to determine how they may affect the treatment plan and what to expect during the procedure.
How to Prepare for Colorectal Cancer Surgery
Prior to surgery, the colorectal surgeon will perform a physical exam, blood tests, and scans to assess the patient's eligibility for the procedure and discuss any risks involved. They will also provide instructions for bowel preparation, such as dietary restrictions or laxatives. Patients are expected to fast for a specified period to ensure an empty stomach during the surgery. Taking certain medications, such as blood thinners, may be temporarily stopped or adjusted to minimise the risk of complications.
Post-Surgery Care for Colorectal Cancer
A comprehensive guide will be provided for patients and their caregivers during the recovery phase after colorectal cancer surgery. As an overall guide, patients are advised to consume small and frequent meals, monitor their weight closely, and avoid taking too many supplements at this stage. Do check with your doctor and nurse care coordinator.
Exercise and Activity
You will be provided with adequate medical leave to rest after surgery. While resting is important, this should be balanced with some daily walks to improve muscle tone, digestion, and mental well-being. Activity is also important to prevent problems such as blood clots in the legs (deep vein thrombosis) and physical deconditioning, especially for the elderly, which can lead to further complications.
We also advise not to commence high-intensity activities too early after colorectal cancer surgery, as these may lead to wound problems such as hernias. A good guide is to wait at least 4-6 weeks before commencing such exercises, and do check with your doctor and nurse care coordinator.
Wound Care
Wound care advice will be provided upon discharge. There may also be a date provided to remove wound sutures or staples with your family physician or by our medical team. In the event of increasing wound pain, redness or some discharge that is unusual, please contact our team for a review.
A stoma is needed in some circumstances after surgery and will be advised. Stomas are usually temporary and are created to divert stools to allow healing of the anastomosis after removal of typically a rectal cancer. This stoma will be closed in a 2nd operation usually after a few months once you have fully recovered. If chemotherapy is required, the stoma is closed only after chemotherapy is completed in order to avoid any delays in your curative treatment.
If the cancer is a very low rectal cancer or involves the anus or anal canal muscles, surgery will require the removal of the anus, making the stoma a permanent one.
Stoma care will be advised and provided by our care team, along with supporting expert vendors. Stoma care will involve ensuring the correct appliances are sized and the type advised based on each individual, and also provide guidance on stoma skin care products.
There will be counselling on overall nutrition and hydration. It is important to regain normal activities of daily living as best even with a stoma and we can provide guidance on how to cope while studying or at work, and also with intimate moments for couples. We will also provide advice on activities such as sports, diving and travel.
FAQ on Colorectal Cancer
Can Colon Cancer be Cured?
What Does Colon Cancer Pain Feel Like?
Is Colon Cancer Fast or Slow Growing?
How Do You Know if it’s Colorectal Cancer or Haemorrhoids (Piles)?
Is Colon Cancer Hereditary?
Helpful Links
Our Colorectal Surgeon

Dr Chew Min Hoe
Medical Director
Senior Consultant, General & Colorectal Surgeon
MBBS (Singapore), MRCS (Edinburgh), MMed (Surgery), FRCS (Edinburgh)
Dr Chew Min Hoe is a colorectal cancer surgeon in Singapore with over 25 years of experience. He has successfully treated numerous cases of colorectal cancer through advanced, minimally invasive procedures and a patient-centred approach.
With a focus on restoring colorectal health, Dr Chew focuses on providing tailored and comprehensive treatment plans for all patients in a supportive environment to ensure optimal cancer clearance and improved outcomes.
Key Publications
Chew MH; Ng KH; Fook-Chong M C Stephanie; Eu KW
Redefining conversion in laparoscopic colectomy and its influence on outcomes: analysis of 418 cases from a single institution.
World journal of surgery 2011; 35(1):178-185
Tan WS; Chew MH; Ooi BS; Ng KH; Lim JF; Ho KS; Tang CL; Eu KW
Laparoscopic versus open right hemicolectomy: a comparison of short-term outcomes.
International journal of colorectal disease 2009; 24(11):1333-9
Chew MH; Wong M TC; Lim B YK; Ng KH; Eu KW
Evaluation of current devices in single-incision laparoscopic colorectal surgery: a preliminary experience in 32 consecutive cases.
World journal of surgery 2011; 35(4):873-880
Lim J WM; Chew MH; Lim KH; Tang CL
Close distal margins do not increase rectal cancer recurrence after sphincter-saving surgery without neoadjuvant therapy.
International journal of colorectal disease 2012; 27(10):1285-1949
Chew MH; Chang MH; Tan WS; Wong M TC; Tang CL
Conventional laparoscopic versus single-incision laparoscopic right hemicolectomy: a case cohort comparison of short-term outcomes in 144 consecutive cases.
Surgical Endoscopy 2013; 27(2):471-477
Tan WJ, Chew MH, Dharmawan AR, Singh M,Acharyya, Loi TT, Tang CL
Critical appraisal of laparoscopic vs open rectal cancer surgery.
World J Gastrointest Surg. 2016 Jun 27;8(6):452-60.
Chew MH, Yeh YT, Lim E, Seow-Choen F.
Pelvic autonomic nerve preservation in radical rectal cancer surgery: changes in the past 3 decades.
Gastroenterol Rep (Oxf). 2016 Aug;4(3):173-85. doi: 10.1093/gastro/gow023. Review.
Tan WJ, Tan HJ, Dorajoo SR, Foo FJ, Tang CL, Chew MH.
Rectal Cancer Surveillance-Recurrence Patterns and Survival Outcomes from a Cohort Followed up Beyond 10 Years.
J Gastrointest Cancer. 2017 Jun 29. doi: 10.1007/s12029-017-9984-z
Our Motto
Caring Hearts, Educated Minds, Skilled Hands
Tel:+65 6518 4688
Fax:+65 6235 0897
Mon-Fri:8:30am - 5:30pm
Sat / PH Eve:8:30am - 12:00 noon
Sun & Public Holiday: Closed
Tel:+65 6518 4868
Fax:+65 6443 6616
Mon-Fri:8:30am - 5:30pm
Sat / PH Eve:8:30am - 12:00 noon
Sun & Public Holiday: Closed


